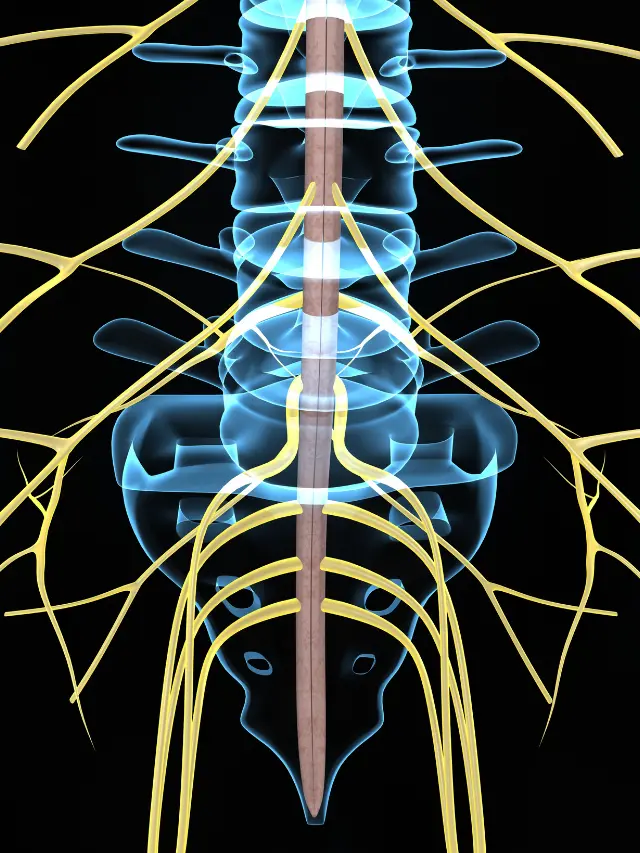
Diabetic neuropathy treatment in Chennai deals with a specific type of nerve damage found in patients with high blood sugar levels (diabetes). Peripheral nerves are commonly affected the peripheral nerves carry motor and sensory signals from the spinal cord to the arms, legs, hands, and feet.
The motor nerve carries motor signals to the muscles and glands. The sensory nerve carries sensory information from the brain to the sensory receptors throughout the body. Damage to the peripheral nerves causes a wide range of symptoms due to the reduced functions of the nerves, Such as the poor ability to feel pain,
Damage to the peripheral nerves causes a wide range of symptoms due to the reduced functions of the nerves, Such as the poor ability to feel pain, changes in temperature, and overall poor sensation in the skin, and joint leading to bone damage over years for many patients.
The autonomic nerves supply internal organs Say lungs, heart liver, kidney, bladder, genitals, digestive glands, etc. The autonomic nervous system controls and regulates body functions like heart rate, respiratory rate, blood pressure, sweat, digestion, urination, and sexual arousal. So inflammation or damage to the peripheral and autonomic nerves causes serious problems that disturb normal day-to-day activities.
Patients with diabetes for a longer period of time have a great risk of diabetic neuropathy. Diabetic neuropathy is common in people who have poor control of blood glucose levels. Peripheral neuropathy is also called distal symmetric neuropathy affects arms and legs.
The diabetic neuropathy treatment in Chennai depends on the symptoms which may vary for the patient from mild to painful and disabling depending upon the severity of the disease.

What is Diabetic Neuropathy?
Diabetic neuropathy is nerve harm that is brought about by diabetes.
Nerves are heaps of exceptional tissues that convey signals between your cerebrum and different pieces of your body. The signs
- send data about how things feel
- move your body parts
- control body works like assimilation
Causes of Diabetic Neuropathy
The significant cause for the development and progression of diabetic neuropathy is poor glycaemic control. (blood glucose level). Diabetic neuropathy treatment in Chennai results due to damage of nerves and blood vessels and the symptoms differ from one person to another according to the type of neuropathy.
High blood sugar weakens the walls of small blood vessels which carry oxygen and nutrients required for the normal day-to-day activities of the body.
Other Causes
- Vitamin B12 deficiency
- Folic acid deficiency
- Smoking
- Alcoholism
- Age-related

Check out Cervical Cancer Prevention, Causes, Symptoms.
Types of diabetic neuropathy
- Peripheral neuropathy
- Autonomic neuropathy
- Proximal neuropathy
- Focal neuropathy
Periphery Neuropathy
Peripheral neuropathy is the commonest form of diabetic neuropathy that affects the nerves in the foot, legs, hands and arms. This type of diabetic neuropathy is called glove and stocking anaesthesia.
Symptoms
The onset of the symptoms is usually from the distal part of the feet to the proximal part of the legs. The patient is diagnosed with the sign of neuropathy on examination but has no symptoms.
- Numbness with reduced or altered sensation
- Pain and weakness of the muscles.
- Loss of reflexes usually in the ankle joint
- Tingling or burning sensation
- Loss of balance and coordination
- Sever foot ulcers with infection
- Foot deformities example hammer toes
- Blisters in numb areas, which when left unnoticed results in injury.
- Sometimes bone and joint pain lead to deformities.
- Increased sensitivity to touch.
Autonomic Neuropathy
Autonomic neuropathy requires an immediate diabetic neuropathy treatment in Chennai because it affects the internal organs such as the cardiovascular system, digestive tract, genital organs, kidneys, bladder day respiratory system which are supplied by autonomic nerves.
Symptoms
- Urinary tract infection
- constipation
- Abdominal Bloating
- Increased or decreased sweating
- Increased heart rate
- Erectile dysfunction
- Vagina dryness
- Visual Disturbances
Proximal Neuropathy
Proximal neuropathy is also called as reticular Plexes neuropathy. This neuropathy affects the nerves in the thighs, hips, buttocks and legs. This neuropathy is common in type 2 diabetes and in old-aged person. This can be called in terms like diabetic amyotrophic, femoral neuropathy and lumbar-sacral plexus neuropathy.
Symptoms
- Severe pain and weakness in hips thighs and lower back region.
- Weak and shrinking thigh muscles.
- Inability to rise from sitting to standing posture.
Mono Neuropathy or Focal Neuropathy
Damage to a specific nerve or a group of nerves due to diabetes affects the face, torso and legs. This type of neuropathy is commonly found in old age people. Focal neuropathy is painful and unpredictable.
It doesn’t cause a long-term effect, symptoms are usually reduced by themselves in weeks or a month. Patients with long-term diabetes or prone to nerve compression called entrapment syndrome, carpal tunnel syndrome leading to tingling sensation in hand and fingers, numbness, and grasping difficulties require prompt diabetic neuropathy treatment in Chennai.
The symptoms of usually pain inside the shin or foot, muscle weakness, lower back pain, pain in the chest and abdomen. Mono neuropathy causes nerve problems leading to difficulty in focus, double vision, and paralysis of one side of the face.
Diagnosis
Nerve conduction study: Electric current is transmitted to the nerve to rule out the damage. Impulses may be slower or weaker depending upon the damage in the nerves.
Electromyography: This studies performed to read the response of the muscle through electric signals. If the response is weak compared to the normal muscle activity it indicates damage to the nerve or muscle.
Quantitative Sensory Testing: The investigation is performed to check the response, to pressure, vibration, temperature and to rule out irritability and sensory loss of the nerves.
Ultrasound: Ultrasound is performed to have a check on internal organs and its functions.
Get detailed info on experience and other credentials of Diabetic neuropathy treatment in Chennai.
Treatment
- Blood Gulcose Control
- Medical Therapy
- Physical Therapy
- Psychological Counselling
Get the best diabetic neuropathy treatment in Chennai from the well experienced VS Multi Speciality Hospitals.
Read also Best Knee Replacement Surgeon in Chennai.